References:
-
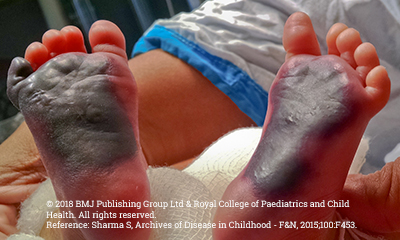
Chalmers E, et al. Purpura fulminans: recognition, diagnosis and management. Archives of Disease in Childhood. 2011;96(11):1066-1071.
-
Price VE, et al. Diagnosis and management of neonatal purpura fulminans. Semin Fetal Neonatal Med. 2011;16(6):318-22.
-
Goldenberg N, Manco-Johnson M. Protein C deficiency. Haemophilia. 2008;14(6):1214–1221.
-
Marlar RA, et al. Report on the diagnosis and treatment of homozygous protein C deficiency. Report of the Working Party on Homozygous Protein C Deficiency of the ICTH-Subcommittee on Protein C and Protein S. Thromb Haemost. 1989;61(3):529-31.
-
Kroiss S, Albisetti M. Use of human protein C concentrates in the treatment of patients with severe congenital protein C deficiency. Biologics: Targets & Therapy. 2010;4:51–60.
C-ANPROM /INT/ /5460- November 2019